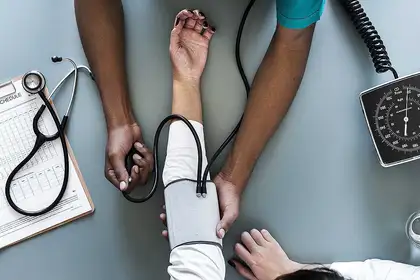
Should consumers be expected to know everything an insurance company requires?
By Dr Micheal Naylor
Fair Go viewers will be familiar with the sad case of Shane Laker, whose insurance company refused to pay out on his income protection policy because he failed to disclose unrelated health conditions.
Shane will be only one of many consumers caught out by insurance application processes that fail to ask specific questions about pre-existing conditions. As we wait for the outcome of the government’s review of insurance law, it seems timely to discuss whether consumers should be expected to know everything an insurance company requires, or whether they should merely be obliged to answer the questions put to them honestly.
In general, the current law allows insurers to ask very few questions at policy creation. There is often very minimal underwriting and non-disclosure issues are not brought to the customer’s attention. It is only at claim time that non-disclosure issues are raised – and then it is too late for the customer to make other insurance arrangements or accept a loading.
One of the reasons for this is, in the past, it was costly to ask questions, it was costly to underwrite, it was costly to offer customised terms, it was costly to gather information, and it was costly to communicate. It was not possible to ask a long list of questions, and it was not possible to modify the questions asked based on responses. It was therefore more efficient to ask detailed questions of the far smaller number of customers who made a claim.

Dr Michael Naylor.
Will insurers really 'look after you'?
Massey University’s research indicates that consumers have little awareness of their disclosure duties and intuitively rely on the advertising promise to ‘look after you’. Consumers think their duty is only to answer questions honestly. When informed of the law, many respond with shock and this contributes to under-insurance.
The UK, after extensive analysis, changed its law so retail consumers are only required to answer the questions asked as accurately and honestly as would be expected of a reasonable respondent, based on what they could be reasonably expected to know. Questions need to be specific and not ‘catch-all’. The insurer is given a set amount of time to ask more questions, after which the policy cannot be cancelled unless false answers were provided.
Despite warnings by UK industry, there have been few difficulties with the new approach, with no change in premiums. The main reason for this is that technology means most consumer contact is now via online systems. Questions can be asked cheaply, and subsequent questions can be added, based on the answers provided. Insurers can also access medical or other databases cheaply if consumers consent.
Technology could make disclosure unnecessary
In the longer term, an increasing number of customers will interact with their insurer via linked telematics. These are devices like Fitbits that allow insurers to set premiums based on ongoing data automatically provided by the customer. This technology allows premiums to be dynamic – for example, car premiums may differ depending on whether the car is being driven or parked. Increasingly, ‘disclosure’ will go from telematic device to insurer algorithm without the knowledge of the insured. The consumer only needs to give permission for this interaction to occur.
Given these developments, the law really should be reformed to place the burden on the knowledgeable party, the insurer, to know what factors are relevant and to ask about them – and to underwrite at policy inception.
A clause requiring consumers to disclose facts that are exceptional and unlikely to be asked by an insurer, and which a reasonable person would know should disclosed, makes sense. The law should be amended to allow a range of remedies, rather than simply cancelling policies, including partial payments.
Finally, an Insurance Conduct Act, outlining a requirement for insurers to respond to claims in a reasonable and timely manner, given the circumstances, would create a fairer playing field between insurers and consumers.
It’s now over to Commerce and Consumer Affairs Minister Kris Faafoi to make the regulatory changes necessary to ensure the problems experienced by Shane Laker don’t continue to plague consumers in the future.
Dr Michael Naylor is an insurance industry researcher at the Massey Business School.